Plantar Fasciitis and Heel Pain PT in Hillsboro, OR
Ligament Rehab • Progressive PT • Structured Load-Based Recovery
Heel pain can make every step frustrating. Whether it hits first thing in the morning, shows up after standing all day, or flares during running and workouts, plantar fasciitis and related heel pain can disrupt training, work, and daily life.
Heel pain that lingers for months is rarely just “inflammation.” Plantar fasciitis often becomes persistent because the tissue’s load tolerance and sensitivity haven’t been restored. Rest may calm symptoms, but progressive loading restores durability.
At Tualatin Valley Physical Therapy, we take a strength-based, movement-focused approach to plantar fasciitis and heel pain. The goal is not just temporary relief; it’s helping you walk, train, and stay active with more confidence and less irritation.
You’ll receive 1-on-1 care with a Doctor of Physical Therapy, with a plan tailored to your activity level, symptoms, and goals.
Common Heel Pain Problems We Treat
Plantar Fasciitis/Plantar Fasciopathy
Pain along the bottom of the heel or arch, often worse:
With the first steps in the morning
After sitting for a while
After long periods of standing
With running, jumping, or increased activity
Achilles/Calf Contribution to Heel Pain
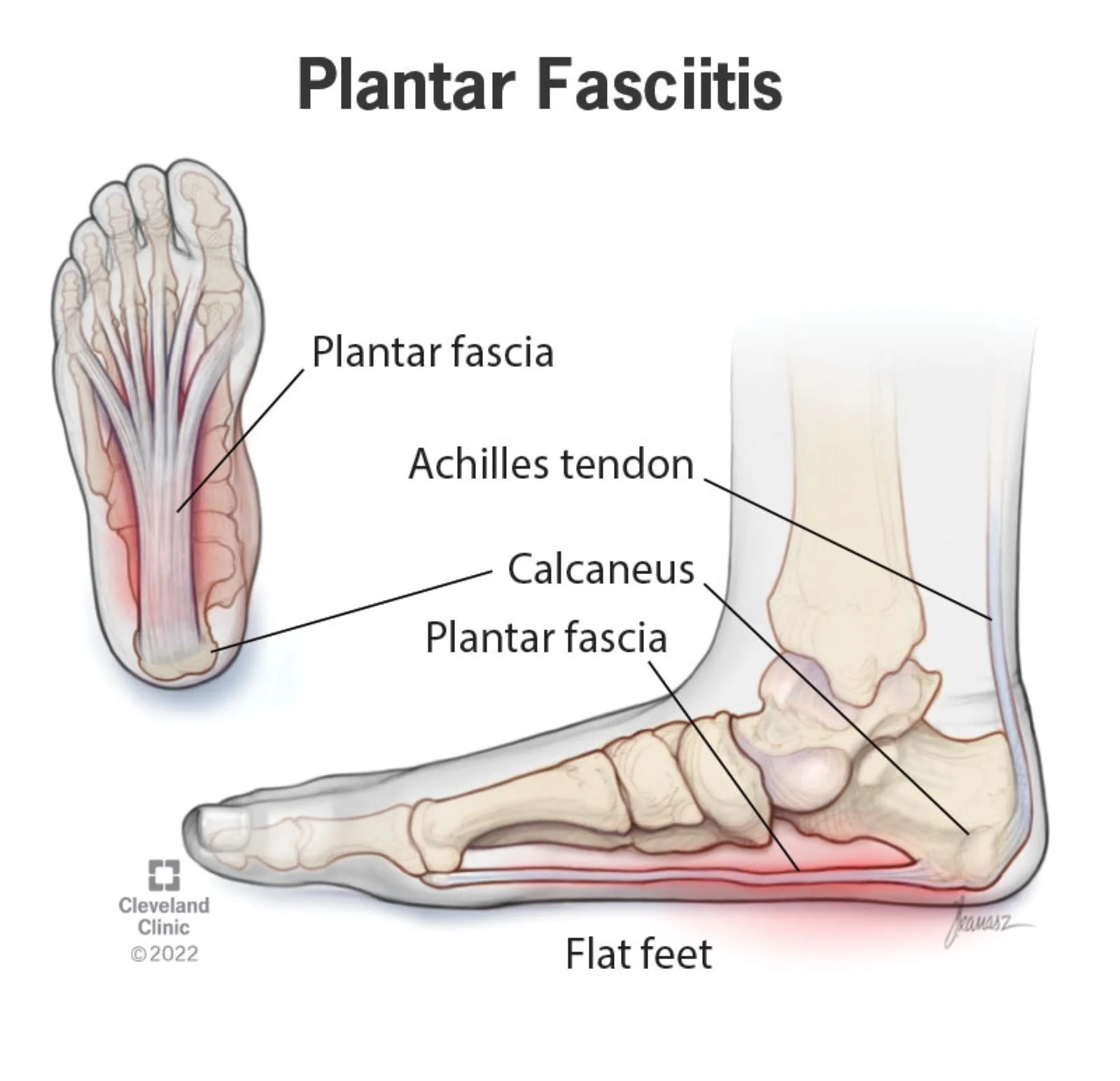
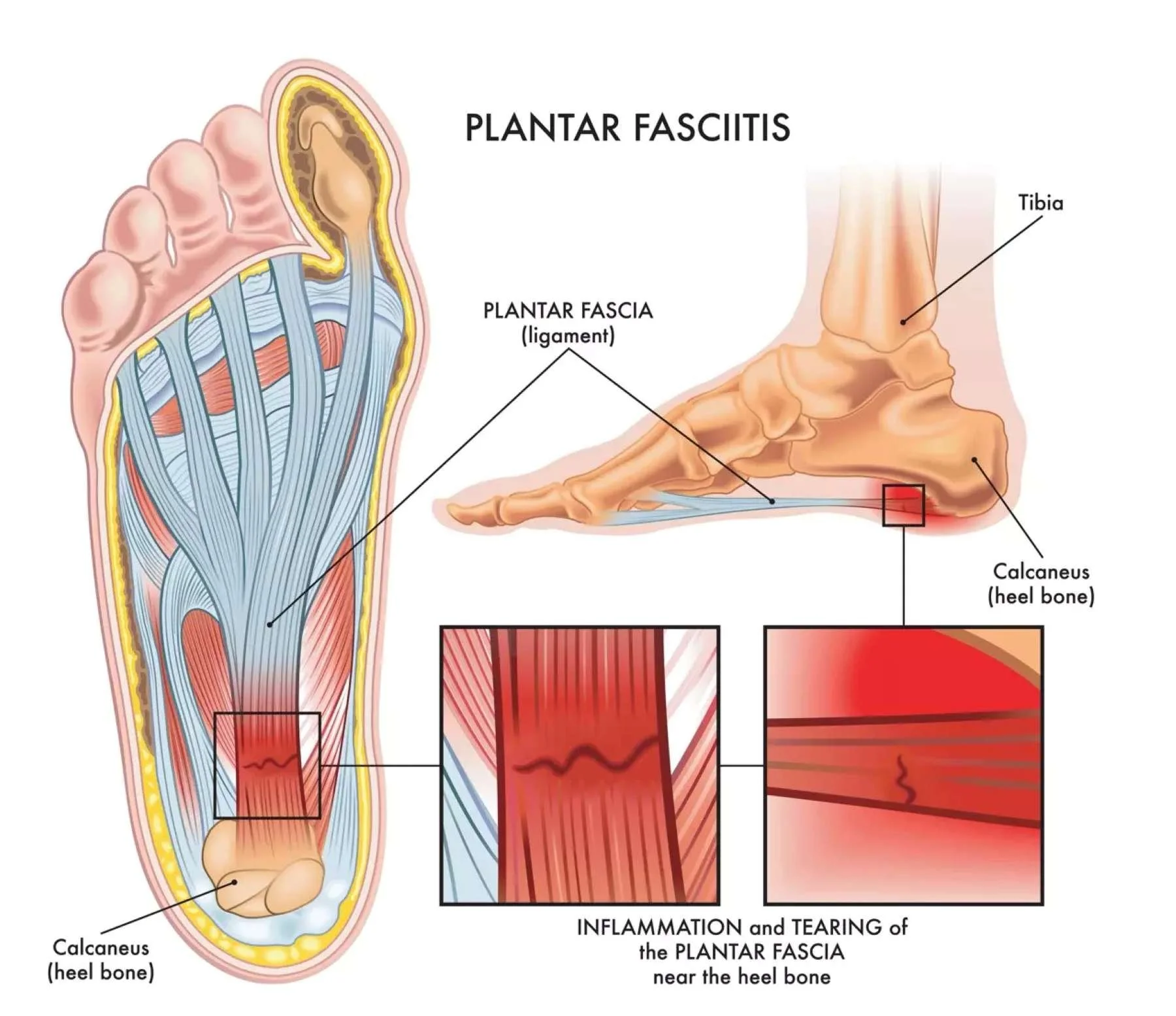
Heel pain is not always just a “foot problem.” Limited calf capacity, ankle stiffness, and tendon overload often contribute to symptoms and recurring flare-ups. For example, flat feet place abnormal stress on the plantar fascia and the Achilles tendon/calf.
What Is Plantar Fasciitis?
The plantar fascia is a thick band of connective tissue that runs along the bottom of your foot and supports the arch.
Plantar fasciitis occurs when this tissue becomes irritated or overloaded, leading to inflammation and pain.
Common symptoms include:
Sharp pain in the heel
Pain with the first steps in the morning
Stiffness after periods of rest
Discomfort after prolonged walking or running
Without proper treatment, plantar fasciitis can become a chronic condition, plantar fasciosis, that lasts for months or even years.
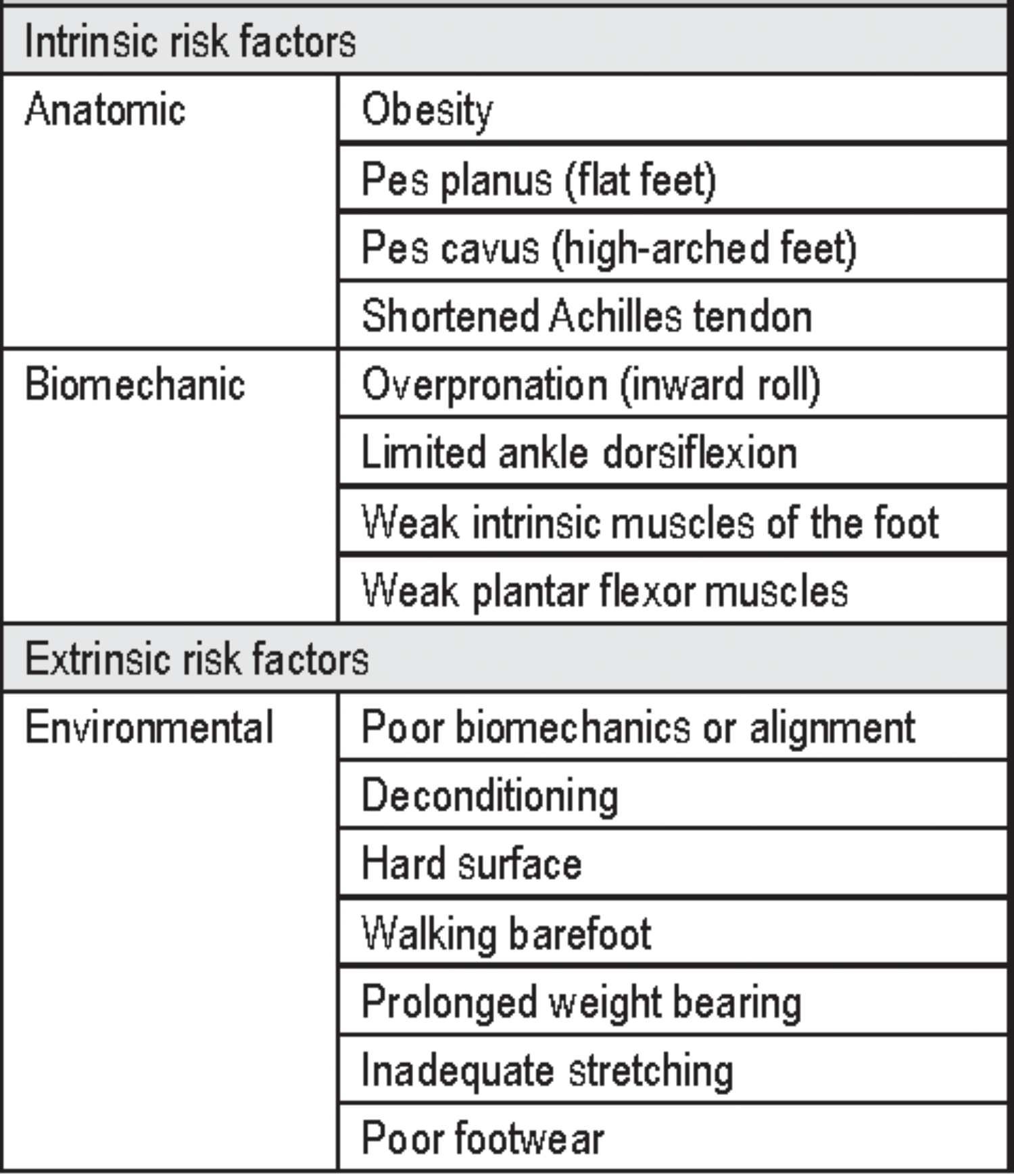
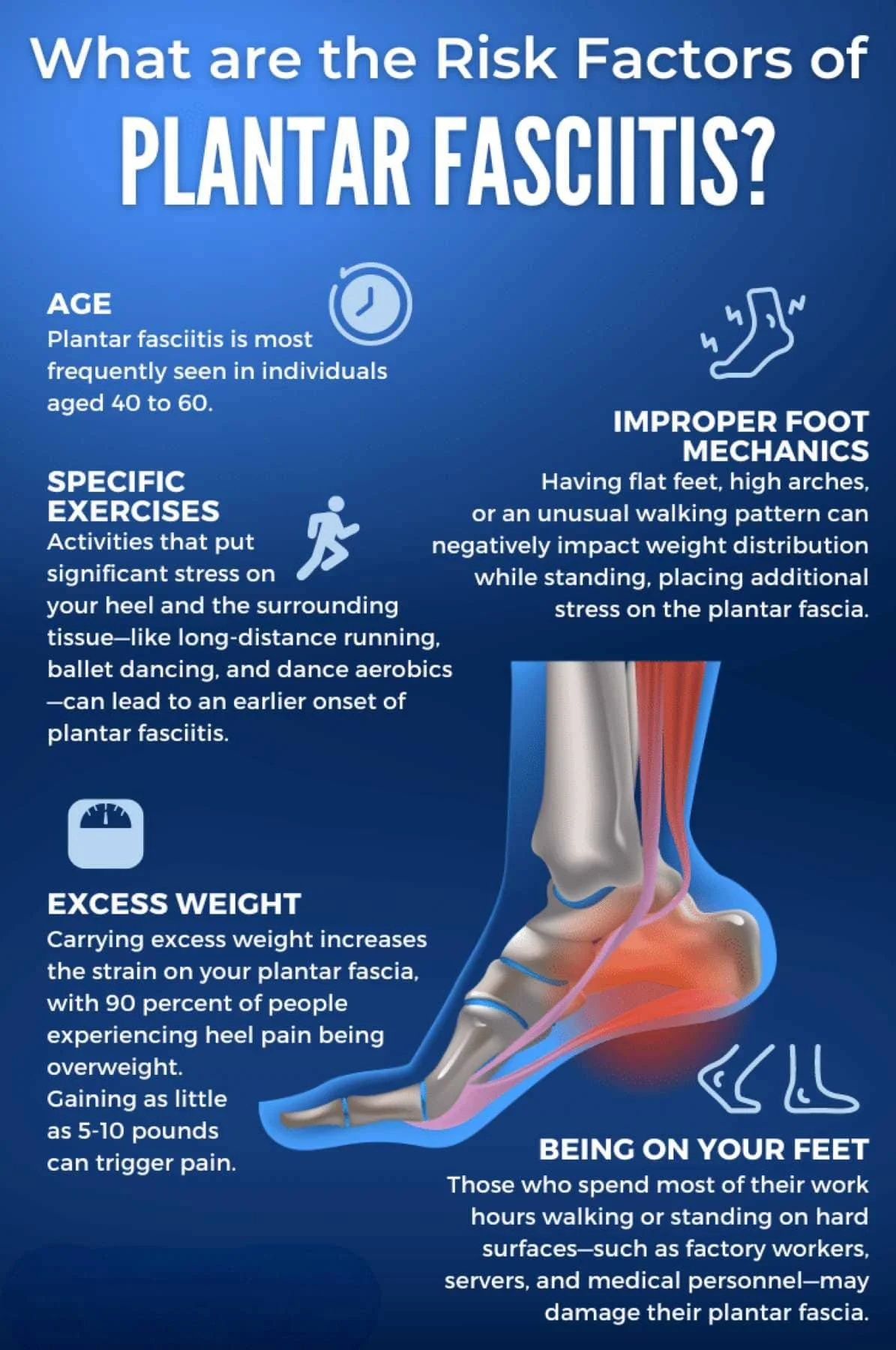
Common Causes of Plantar Fasciitis
Several factors can contribute to the development of plantar fasciitis.
These include:
Sudden increases in running or exercise
Prolonged standing or walking
Poor footwear support
Limited ankle mobility
Calf muscle tightness
Foot mechanics and arch structure
A detailed physical therapy evaluation helps identify which factors are contributing to your symptoms.
How Physical Therapy Helps Plantar Fasciitis
Physical therapy is one of the most effective treatments for plantar fasciitis because it addresses the root causes of heel pain.
Treatment may include:
Targeted strengthening exercises
Calf and foot mobility work
Manual therapy
Gait and movement analysis
Progressive loading of the plantar fascia
These interventions help improve tissue resilience and reduce strain on the plantar fascia.
Chronic Plantar Fasciitis or Heel Pain
Why Heel Pain Keeps Returning
If you’ve had heel pain for months or it keeps returning whenever activity increases, there is usually an underlying issue that hasn't been fully addressed.
Many people cycle through:
Icing
Orthotics
Injections
And other forms of temporary relief
But the pain keeps returning with activity.
Pain ≠ damage alone.
Pain often reflects tissue sensitivity.

The Real Reason Heel Pain Returns
Plantar fasciitis often becomes persistent when the tissues at the bottom of the foot are being asked to tolerate more load than they’re prepared for.
Common reasons it keeps returning:
Calf and foot strength haven’t been rebuilt
Ankle mobility is limited
Walking, standing, or running volume increased too quickly
Footwear changes altered loading
Rehab focused only on stretching and rest
Symptoms improved temporarily, but tissue capacity never caught up
We focus on improving how your foot and ankle handle load, not just calming symptoms for a few days.
Our Treatment Approach
1) Identify what’s actually driving the pain
We look at:
Symptom pattern and irritability
Walking and standing tolerance
Calf strength and endurance
Ankle mobility
Foot loading mechanics
Training, work, and daily movement demands
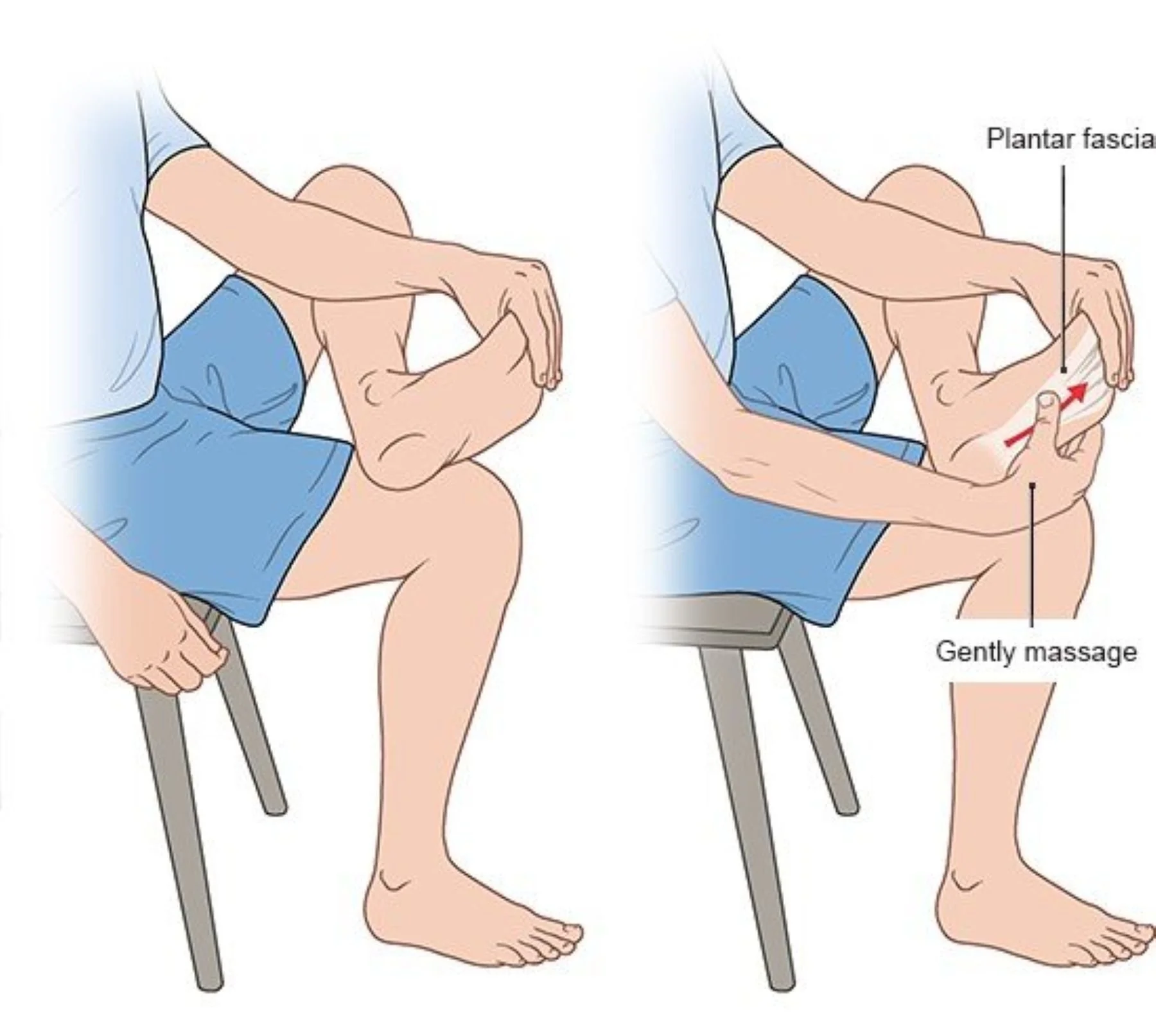
3) Rebuild strength and load tolerance
Treatment may include:
Progressive calf strengthening
Foot and ankle loading progressions
Mobility work when appropriate
Manual therapy when appropriate
Return-to-walking and return-to-running progressions
Guidance on footwear changes when relevant

2) Reduce irritation without shutting your life down
You’ll get clear guidance on:
How to modify an activity without complete rest
What to do when symptoms flare
How to improve tolerance for walking, standing, exercise, and work demands
4) Return to activity with confidence
Whether your goal is to:
Walk comfortably
Work on your feet without pain
Return to lifting
Get back to running
Stay active without recurring flare-ups
…your plan is built around those outcomes.
Especially Helpful For
Runners and active adults
People on their feet for work
Gym-goers and recreational athletes
Hikers and walkers
Anyone dealing with stubborn heel pain that keeps coming back
Advanced Treatment Options for Chronic Heel Pain
Many patients with chronic plantar fasciitis benefit from advanced treatments such as Shockwave Therapy (SWT) and High-Intensity Laser Therapy (HILT) when traditional care has not resolved symptoms. If plantar fasciitis or heel pain has persisted for several months, advanced therapies may help stimulate healing.
At Tualatin Valley Physical Therapy, we offer:
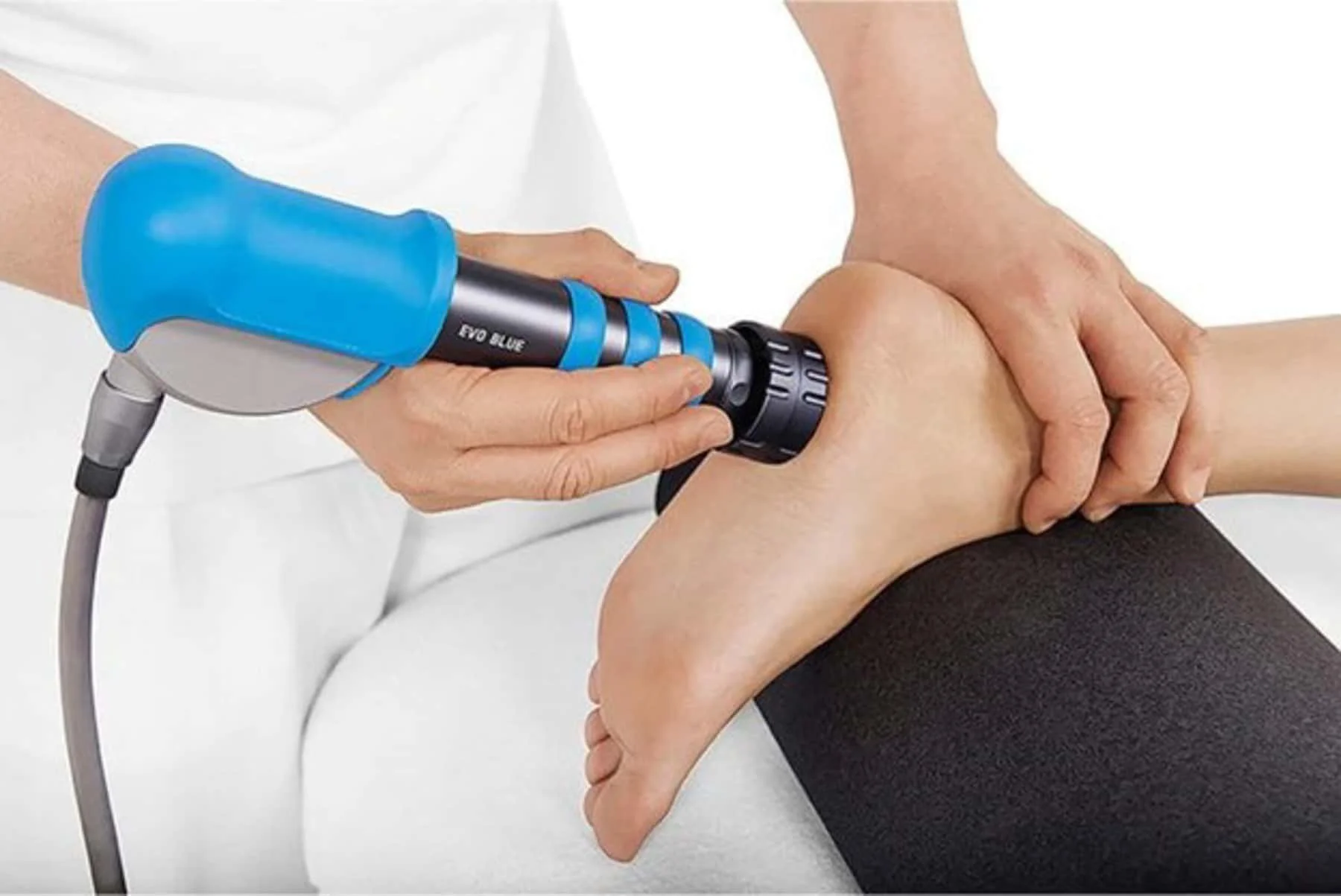
Shockwave Therapy
Shockwave Therapy uses acoustic pressure waves to stimulate healing in chronic tendon and fascia injuries.
Research suggests shockwave therapy can help:
Increase blood flow
Stimulate collagen production
Restart stalled healing processes
Learn more about Shockwave Therapy →
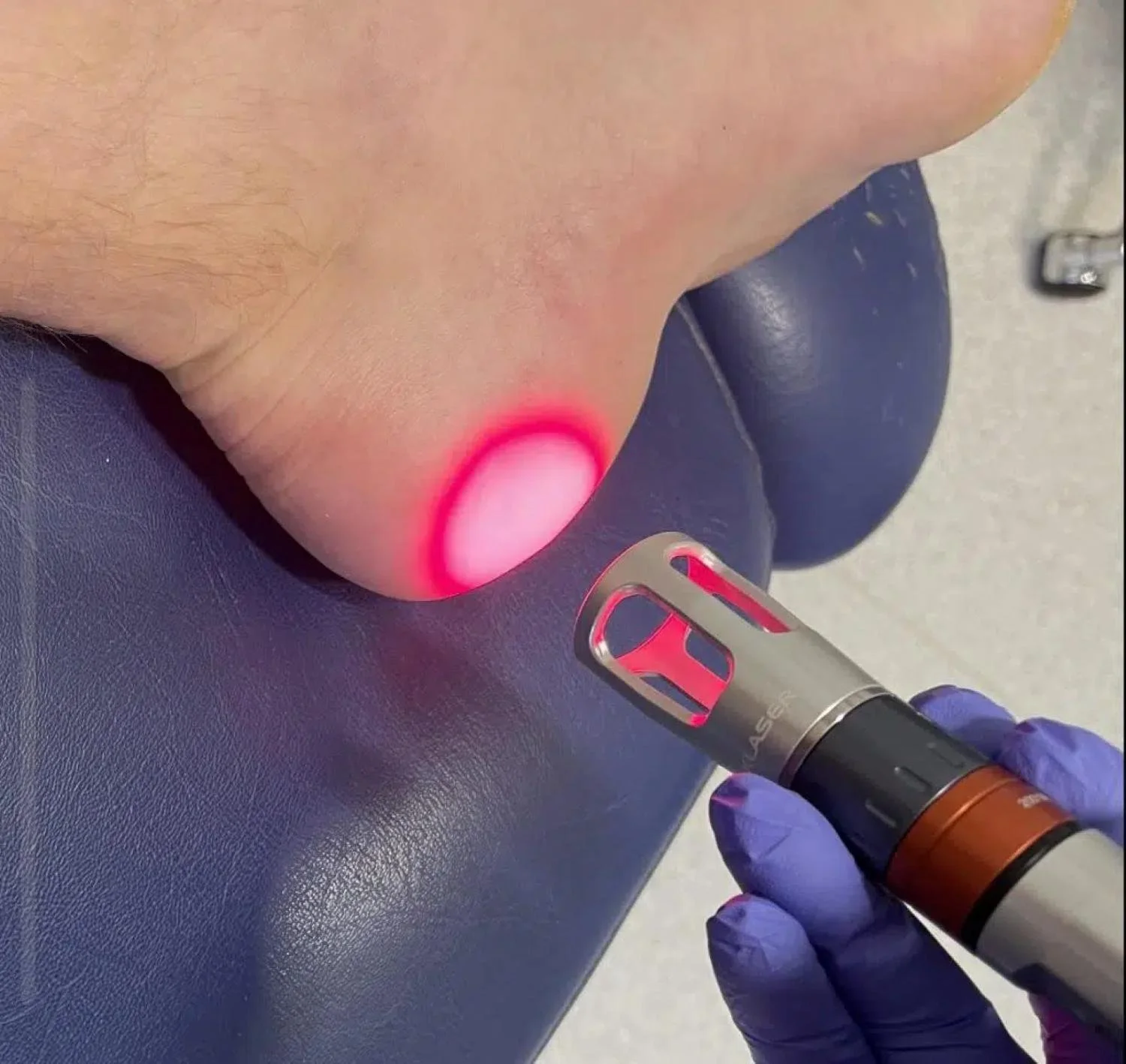
High-Intensity Laser Therapy
High-Intensity Laser Therapy uses light energy to stimulate cellular repair and reduce inflammation.
Laser therapy may help:
Reduce pain
Improve circulation
Accelerate tissue healing
Learn more about Laser Therapy →
Accelerated Recovery Frequently Asked Questions
-
The most effective approach usually includes a combination of targeted strengthening exercises, mobility work, and activity modification. In some cases, advanced treatments such as shockwave therapy may help accelerate healing.
-
Some mild cases improve with rest and stretching, but many cases persist without proper treatment. Addressing underlying movement and loading issues is often necessary for long-term relief.
-
Shockwave therapy is commonly used for chronic plantar fasciitis that has not responded to other treatments. It works by stimulating the body’s natural healing response in the plantar fascia.
-
High-intensity laser therapy may be used to support pain modulation and improve tolerance to structured rehabilitation. It is typically integrated with progressive loading rather than used as a standalone treatment.
-
We select radial shockwave, focused shockwave, or both, depending on the case. Radial shockwave often fits broader, more superficial targets, while focused shockwave may be used when greater precision or deeper targeting is needed.
What to Expect at Your First Visit
Your evaluation includes:
1-on-1 assessment with a Doctor of Physical Therapy
Symptom and activity review
Strength, mobility, and load tolerance testing
Walking and movement assessment
A clear plan of care with next-step recommendations
Exercises that actually match your goals and schedule
You’ll leave with a plan that makes sense, not just generic stretches.
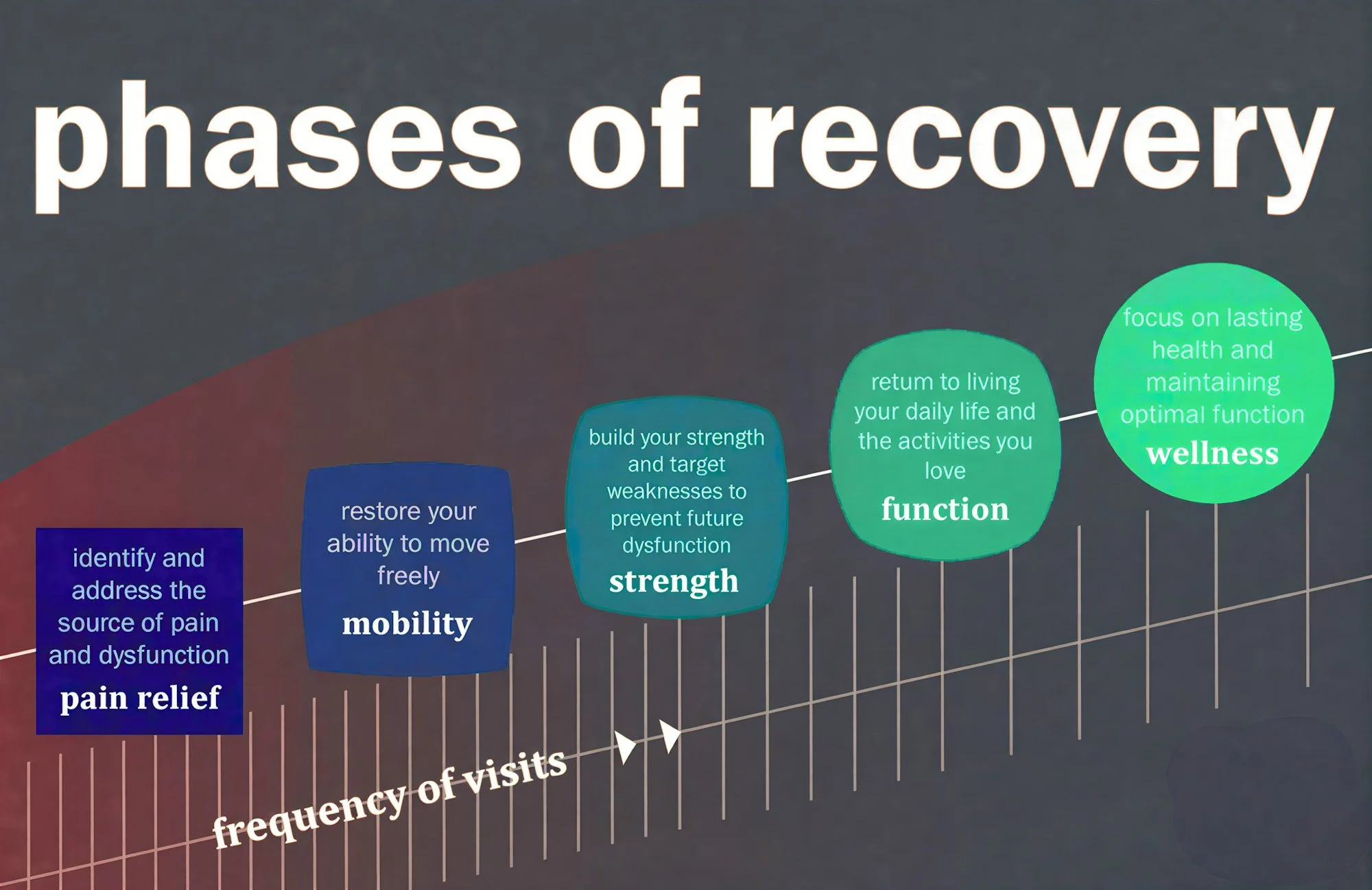

What Recovery Typically Looks Like
Most cases involve:
✔ Symptom stabilization
✔ Strength development
✔ Gradual load exposure
✔ Movement enhancement
✔ Multi-session progression
We avoid passive-only care cycles.
Why Choose Tualatin Valley Physical Therapy?
Unlike high-volume clinics, every visit at TVPT includes:
✔ One-on-one care with a Doctor of Physical Therapy
✔ Personalized treatment plans
✔ Movement analysis and rehabilitation
✔ Evidence-based treatment methods
✔ Rehab based on YOUR goals
Our goal is to help you return to the activities you enjoy without persistent pain.
When Should You Seek Treatment?
You may benefit from physical therapy if:
Heel pain has lasted longer than two weeks
Symptoms worsen with activity
Morning heel pain is severe
Previous treatments have not resolved the problem
Early treatment can often prevent plantar fasciitis from becoming chronic.
If you are experiencing heel pain or plantar fasciitis, a personalized physical therapy evaluation can help identify the cause and guide an effective treatment plan.
Plantar Fasciitis Frequently Asked Questions
-
Plantar fasciitis usually causes pain at the bottom of the heel or along the arch. It is often worse with the first few steps in the morning, after sitting, or after prolonged standing or activity.
-
Not always. Many persistent cases involve a mismatch between tissue tolerance and the loads being placed on it. Pain can also reflect sensitivity and irritation rather than active inflammation alone.
-
Recovery time varies. Some cases improve within several weeks, while more stubborn cases can take longer. The timeline often depends on the tissue's level of irritation, how long symptoms have been present, and whether strength and load tolerance are being rebuilt.
-
You should get evaluated if heel pain has lasted more than a couple of weeks, keeps recurring, limits walking or exercise, or affects work and daily activities.
-
It depends on irritability, chronicity, and how your tissue responds to progressive loading. Many plans involve multiple visits over several weeks with a structured progression rather than a one-size-fits-all timeline.
-
Sometimes, yes. It depends on symptom severity, irritability, and how symptoms respond to loading. Many runners do best with temporary modifications rather than stopping completely.
-
Usually, some walking is still okay, but the amount may need to be modified based on your symptoms. A clinician can help you determine how much is helpful versus how much is too much.
-
Stretching can be helpful for some people, but it often isn’t sufficient on its own for persistent cases. We focus on restoring load tolerance and capacity through structured rehabilitation and progressive strengthening.
Ready to Start Moving With Less Heel Pain?
If plantar fasciitis or heel pain is limiting your job, workouts, or daily life, the next step is getting a clear plan.
Stop Waiting. Start Recovering.
No referrals. No insurance delays. No techs or aides.
Just one-on-one care with a Doctor of Physical Therapy.
Whether you’re dealing with back pain, a sports injury, an auto accident, or a work injury, we make it simple to get started. Same-day appointments available.
Serving Hillsboro, Cornelius, Forest Grove, Aloha, North Plains, and the greater Tualatin Valley.
Call us today at (971) 238-5755, or click the button below to schedule your initial evaluation online.
Unsure if self-pay physical therapy is for you? Schedule a free 15-minute consultation using the same button!
Our friendly team is ready to guide you on your path to recovery and lasting wellness.
Auto (PIP) Accepted
〰️
Workers' Compensation Accepted
〰️
Out-of-Network Reimbursement Available
〰️
Auto (PIP) Accepted 〰️ Workers' Compensation Accepted 〰️ Out-of-Network Reimbursement Available 〰️
Transparent pricing. Clear plan. No surprise bills.
Experience the TVPT Difference.


