How Long to Rest an Injury: A Guide to Optimal Recovery Time
When you sustain an injury, the immediate impulse is often to "rest it out." This common adage, however, frequently oversimplifies a complex biological process. While rest is a crucial component, understanding how long to rest an injury and what constitutes optimal recovery is far more nuanced than simple inactivity. Modern approaches emphasize a proactive, science-backed strategy that balances rest with controlled movement and rehabilitation.
This guide delves into the science of healing, explores evolving recovery protocols, and provides a framework for personalizing your journey back to full health and activity, whether you're an athlete or simply navigating daily life.
Beyond Just "Resting It Out"
The instinct to immobilize an injured body part is deeply ingrained, largely stemming from older medical advice. However, this approach often overlooks the dynamic nature of healing. Private industry employers reported 2.6 million nonfatal workplace injuries and illnesses in 2023, of which 946,500 involved days away from work [U.S. Bureau of Labor Statistics, 2023].
This highlights the significant impact injuries have on our ability to function. Understanding how long to rest an injury means moving beyond passive waiting and embracing a strategy that actively promotes tissue repair and functional restoration.
The Common Misconception About Injury Recovery
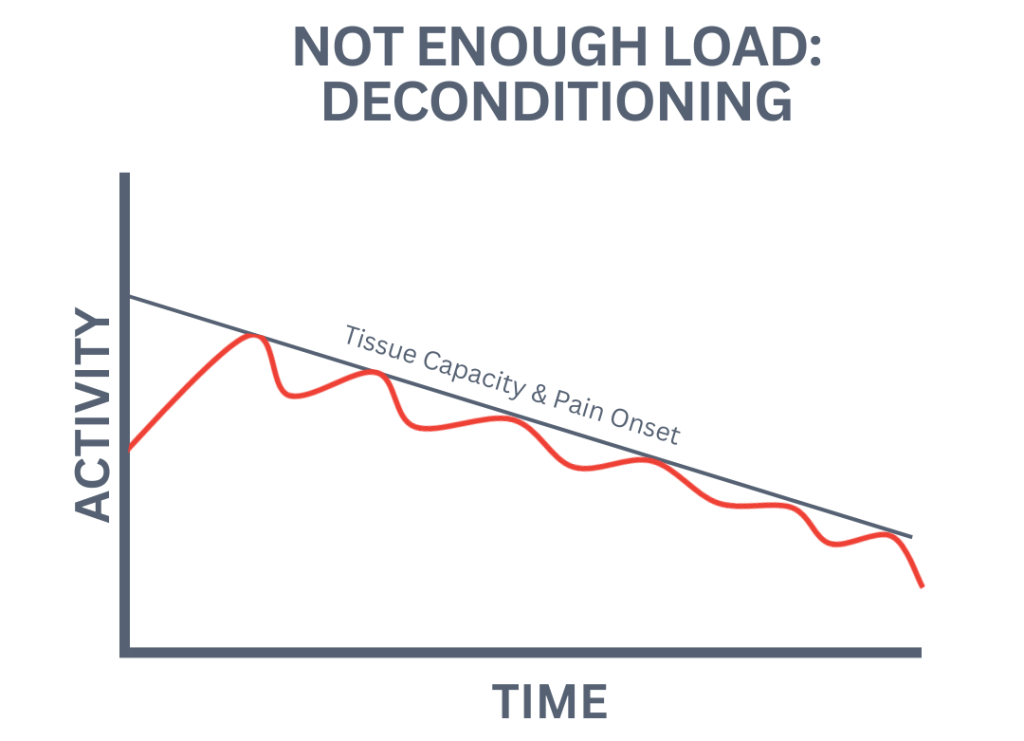
For decades, the prevailing wisdom for managing an injury was to cease all activity and allow the body time to heal passively. This often translates to prolonged periods of inactivity, which, while seemingly logical, can sometimes impede the recovery process. This misconception fails to acknowledge that tissues, under appropriate stress, can adapt and strengthen. Complete cessation of activity can lead to deconditioning, muscle atrophy, and joint stiffness, potentially prolonging the overall recovery timeline.
What Optimal Recovery Really Means: A Proactive Approach to Healing
Optimal recovery is not about achieving the shortest possible downtime but about facilitating the most complete and robust healing. It's a proactive, multi-faceted process that involves understanding the injury, respecting the body's healing phases, and strategically reintroducing stress to promote adaptation. This approach prioritizes restoring full function, strength, and resilience to prevent reinjury. It is a journey guided by science and tailored to the individual.
Why a "One-Size-Fits-All" Timeline Doesn't Work
Every injury is unique, influenced by the type of tissue damaged, the severity of the trauma, and individual biological factors. A mild ligamentous sprain will demand a different recovery path than a significant muscle tear. Furthermore, an athlete's demands differ vastly from those of someone recovering from an injury sustained during daily activities. Age, overall health, nutritional status, and lifestyle all play significant roles. Therefore, a universal timeline for injury recovery is not only impractical but potentially detrimental, leading to either premature return to activity or unnecessary prolonged rest.
Understanding Your Injury: The Foundation of Recovery
Before any effective recovery plan can be formulated, a thorough understanding of the injury itself is paramount. This involves identifying the specific tissues involved, the extent of the damage, and the overall context of the injury.
Types of Injuries and Their Basic Recovery Needs
Injuries can be broadly categorized as acute (sudden-onset, such as a sprain or strain) or chronic (developing over time due to repetitive stress). Sprains and strains account for approximately 30% of all sports injuries [Market.us Media, 2025], impacting ligaments and muscles, respectively. Soft tissue injuries, which include muscles, tendons, and ligaments, require specific attention to promote cellular repair and regain elasticity.
The Critical Role of a Professional Diagnosis
Self-diagnosing an injury can be inaccurate and lead to ineffective or even harmful treatment. A medical professional, such as a Doctor of Physical Therapy, can accurately identify the injured tissue, assess its severity, and rule out more serious conditions. This diagnosis forms the bedrock of a tailored recovery plan, ensuring that the treatment aligns with the specific pathology. Ignoring professional advice can lead to complications and a prolonged recovery period.
Injury Severity: Why Grading Matters for Recovery Timelines
Injuries are often graded by severity, particularly sprains and strains. A Grade I injury involves a mild stretch or tear, Grade II a moderate tear, and Grade III a complete rupture. For instance, hamstring strains, a common sports injury, can have vastly different recovery timelines depending on their grade. A complete hamstring tear (Grade III) might require surgical intervention and a recovery period extending up to a year. In contrast, a Grade I strain might only necessitate a few weeks of modified activity [Adam Loiacono, 2025]. Understanding this grading is essential for setting realistic recovery expectations.
The Science of Healing: What Happens Inside Your Body
The process of healing is a complex biological cascade, orchestrated by the body to repair damaged tissue and restore function. Understanding these phases provides crucial insight into why certain interventions are recommended at different stages.
The Three Phases of Tissue Healing
Tissue healing typically progresses through three overlapping phases:
Inflammation Phase (0-4 days): Immediately following injury, the body initiates an inflammatory response. This involves increased blood flow to the area, bringing vital cells and nutrients to initiate cleanup and repair. While this phase can cause pain and swelling, it is a critical and necessary step.
Proliferation Phase (4-21 days): In this phase, new tissue begins to form. Fibroblasts produce collagen, which acts as a scaffolding for the new tissue. Blood vessels also regrow to supply the healing area. This is when the injured tissue starts to regain some of its strength.
Remodeling Phase (21 days to several months/years): This is the longest phase, where the newly formed tissue is strengthened and reorganized to resemble the original tissue. Collagen fibers realign along lines of stress, improving the tissue's tensile strength and durability.
How Different Tissues Heal: Implications for Recovery Time
Different types of tissue have varying blood supplies and cellular structures, which influence their healing capacity and speed. Muscles and skin, with good blood supply, tend to heal relatively quickly. Ligaments and tendons have a poorer blood supply, meaning they often take longer to repair. Joints, which contain cartilage, have a very limited blood supply, making injuries to these structures particularly slow to heal and prone to long-term complications. This differential healing rate underscores the need for a varied approach to recovery.
The "Why" Behind Rest and Load: Optimizing Tissue Repair
While rest is important to protect acutely injured tissue from further damage, complete inactivity can hinder healing. Controlled mechanical stress, or "load," is crucial during the proliferation and remodeling phases. Applying appropriate load stimulates cells to produce collagen and helps align it efficiently, leading to stronger, more resilient tissue. Without this stimulus, scar tissue can be disorganized and weak. The key is finding the right balance between sufficient rest to prevent aggravation and enough controlled activity to promote healing.
Evolving Beyond RICE: Introducing PEACE & LOVE for Modern Recovery
For years, the R.I.C.E. (Rest, Ice, Compression, Elevation) protocol dominated injury management. While it offers some benefits, particularly in the immediate aftermath, modern understanding emphasizes a more active and comprehensive approach.
The Traditional R.I.C.E. Protocol: History, Benefits, and Limitations
R.I.C.E. was designed to reduce pain and swelling in the acute phase of an injury. Rest limits further damage; ice constricts blood vessels to reduce swelling; compression minimizes fluid accumulation; and elevation aids drainage. However, prolonged rest can have adverse effects, and an emphasis solely on reducing inflammation may actually impede the early stages of tissue repair. Ice, while effective for short-term pain relief, can also blunt the necessary inflammatory response and delay recovery.
P.E.A.C.E.: Immediate Post-Injury Management
The P.E.A.C.E. protocol offers guidance for the initial 24-72 hours post-injury:
Protection: Avoid movements and activities that increase pain for the first 1-3 days.
Elevation: Keep the injured limb elevated above the heart to help reduce swelling.
Avoid Anti-inflammatories: While pain relievers might be tempting, non-steroidal anti-inflammatory drugs (NSAIDs) may hinder tissue healing. Natural anti-inflammatory processes are crucial.
Compression: Apply a compression bandage to limit excessive swelling and bruising.
Educate: Understand your injury and the recovery process. Empower yourself with knowledge and focus on active recovery strategies when pain allows.
L.O.V.E.: Long-Term Recovery and Active Rehabilitation
Following the initial P.E.A.C.E. phase, the L.O.V.E. protocol guides the subsequent recovery and rehabilitation:
Load: Gradually and progressively load the injured tissues. This means reintroducing controlled activity and exercises that challenge the healing tissue without causing excessive pain.
Optimism: Maintain a positive outlook. Psychological factors significantly influence recovery outcomes.
Vascularization: Engage in pain-free cardiovascular activity to increase blood flow to the injured area, promoting healing.
Exercise: Restore mobility, strength, and proprioception through a tailored exercise program. This is the core of active rehabilitation.
The Core Principle: Load Management, Not Just Rest
The most significant paradigm shift in injury recovery is the understanding that strategic loading, rather than complete inactivity, is often the key to optimal healing.
Strategic Rest vs. Complete Inactivity: The Balance for Tissue Healing
Strategic rest involves modifying your activity to avoid aggravating the injury, not necessarily ceasing all movement. Complete inactivity can lead to muscle atrophy, joint stiffness, and decreased bone density. Controlled loading, conversely, provides the mechanical stimulus needed for tissues to remodel and strengthen, facilitating a faster and more robust recovery. The goal is to find the "sweet spot" where the body is challenged enough to promote healing without causing further damage.
The Dangers of the "Boom and Bust" Cycle
A common pitfall in recovery is the "boom and bust" cycle. This occurs when individuals experience a few pain-free days and drastically increase their activity levels, only to reinjure themselves. This is followed by another period of rest, repeating the cycle. This pattern is detrimental because it constantly disrupts the healing process, leading to chronic pain and longer recovery times. Progressive overload, gradually increasing the demands on the injured tissue, is the antidote to this cycle.
Decoding Pain: When to Push, When to Pause
Pain is a signal, but not always a definitive stop sign. During rehabilitation, it's often beneficial to work with a low level of symptoms, typically around a 3 out of 10 on a pain scale, as long as the pain does not increase significantly during or after the activity and resolves quickly afterward [Central Performance]. Pain that is sharp, intense, or persists for hours after activity usually indicates that the load is too high and should be reduced. Learning to differentiate between "good" soreness and "bad" pain is a crucial skill for effective recovery.
Gradual Return to Activity and Progressive Overload
The return to full activity must be a gradual, step-by-step process. This involves progressive overload, where the demands placed on the healing tissue are systematically increased over time. For example, after a hamstring strain, one might progress from gentle stretching to bodyweight exercises, then to light resistance training, and finally to sport-specific drills. This phased approach ensures that the tissue is adequately conditioned to handle the stresses of full activity, significantly reducing the risk of reinjury.
Personalizing Your Recovery Timeline: It's Not One-Size-Fits-All
The duration of an injury recovery is highly variable. Recognizing the factors that influence this timeline allows for a more realistic and effective rehabilitation plan.
Key Factors Influencing Recovery Duration
Several factors dictate how long it takes to recover from an injury. These include:
Type and Severity of Injury: A muscle strain will heal differently from a ligament tear, and a Grade I injury will resolve faster than a Grade III.
Location of Injury: Tissues with better blood supply heal faster.
Age and Overall Health: Younger individuals and those with better general health tend to recover more quickly.
Adherence to Rehabilitation Program: Consistent and correct execution of the prescribed exercises is critical.
Previous Injury History: Scar tissue from previous injuries can sometimes affect healing.
The Profound Impact of Lifestyle on Tissue Healing
Beyond the immediate injury, lifestyle factors play a monumental role in the body's ability to heal.
Nutrition: Adequate protein intake is essential for tissue repair and collagen synthesis. Vitamins like C and D, and minerals like zinc, are also vital for wound healing. Staying well-hydrated supports all bodily functions, including healing.
Sleep: Sleep is when the body undertakes significant repair and regeneration. Chronic sleep deprivation can impair immune function and slow down the healing process. Aiming for 7-9 hours of quality sleep per night is non-negotiable for optimal recovery.
Stress Management: High levels of chronic stress can increase inflammation and suppress the immune system, negatively impacting the body's ability to heal. Techniques like mindfulness, meditation, or engaging in enjoyable, low-impact activities can help manage stress.
Your Active Recovery & Rehabilitation Plan: A Phased Approach
A well-structured rehabilitation plan is the cornerstone of effective injury recovery, guiding you through distinct stages of healing and functional restoration.
Early Stage Rehabilitation: Gentle Movement and Range of Motion
In the immediate aftermath of an injury, once the acute inflammation begins to subside (often after 24-72 hours, guided by the P.E.A.C.E. principles), the focus shifts to gentle movement. This stage aims to restore pain-free range of motion, prevent stiffness, and maintain circulation to the injured area. Exercises are typically low-impact and pain-free.
For example, gentle ankle circles or passive knee flexion might be used for a lower-limb injury.
Mid-Stage Rehabilitation: Building Strength and Endurance
As pain subsides and range of motion improves, the rehabilitation program progresses to building strength and endurance in the injured tissues and surrounding muscles. This phase involves introducing resistance exercises, both isometric (muscle contraction without joint movement) and isotonic (muscle contraction with joint movement). Proprioception (balance and joint position sense) exercises are also crucial here.
For a knee injury, this might include controlled squats, lunges, or balance exercises on unstable surfaces.
Late Stage Rehabilitation: Functional Movement and Return to Activity
The final stage focuses on restoring full functional capacity and preparing the individual to return to their desired activities, whether that's sports, work, or daily life. This involves sport-specific drills, plyometrics (explosive movements), and higher-intensity conditioning.
The goal is to ensure the injured tissues can withstand the demands of the activity without pain or risk of reinjury. This stage requires careful progression and often involves mimicking the movements and stresses of the intended activity.
Typically, this is when insurance stops covering your visits. To progress beyond the bare minimum and bridge the gap between rehab and performance, many will benefit from boutique-style physical therapy.
The Indispensable Role of a Physical Therapist/Physiotherapist
Throughout all stages of recovery, the guidance of a physical therapist (PT) or physiotherapist is invaluable. They possess the expertise to accurately diagnose injuries, design personalized rehabilitation programs, and monitor progress.
A PT can identify subtle biomechanical issues, prescribe appropriate exercises, provide manual therapy, and guide the gradual return to activity, significantly optimizing recovery time and reducing the risk of setbacks. Consulting a professional minimizes rest and maximizes recovery potential.
Embrace the Journey
Determining how long to rest an injury is a dynamic process, not a fixed endpoint. It requires a departure from the old adage of simply "resting it out" and an embrace of a proactive, evidence-based approach.
Understanding the science behind tissue healing, moving beyond outdated protocols like RICE to embrace P.E.A.C.E. and L.O.V.E., and prioritizing strategic load management are fundamental.
Personalizing your recovery timeline by considering all the factors that influence it, especially crucial lifestyle elements like nutrition, sleep, and stress, empowers you to take control.
Ultimately, a phased approach to rehabilitation, guided by professional expertise, is the most effective path not just to healing but to achieving full, resilient function and preventing future injuries. Embrace the journey with patience, persistence, and a commitment to intelligent recovery.
Are you ready for personalized, one-on-one care to optimize your recovery?
Click here to book your appointment online.